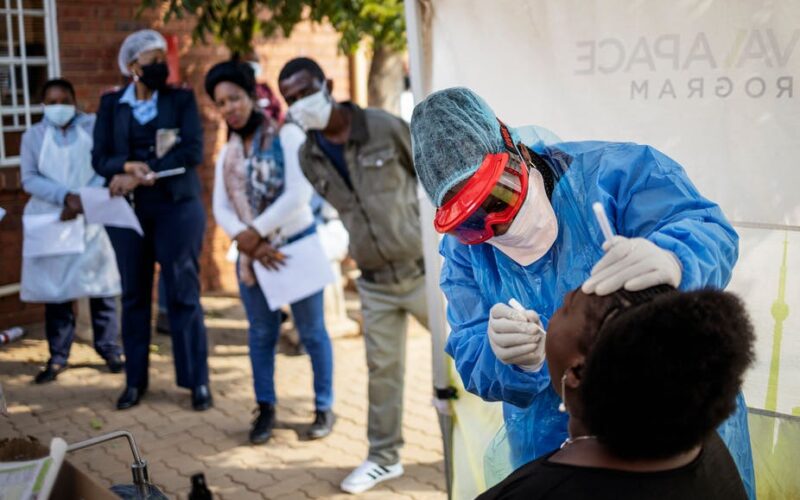
AS the COVID-19 pandemic escalates, South Africa is struggling to keep up with the demand for testing. This has pushed laboratory professionals and clinicians to consider using alternative tests that are commonly used to diagnose and detect exposure to other viral infectious diseases. The Conversation Africa’s Ina Skosana asked Professor Eftyhia Vardas to explain what’s being done.
What’s the most commonly used test?
Polymerase chain reaction (PCR) tests are the standard means of diagnosing viral respiratory infections. It is a molecular test that detects the viral genetic material that indicates the presence of the actual virus, SARS-CoV-2, that causes COVID-19. PCR tests remain the standard diagnostic test for symptomatic individuals.
The tests are very sensitive, detecting minuscule amounts of viral genetic material (RNA) in a sample. Probes are designed to recognise and identify specific regions of the viral genetic material needed to confirm the presence of the virus. Samples may be taken either as a throat swab through the mouth (oropharyngeal) or through the nose (nasopharyngeal) or just of the nose (nasal).
What are the shortfalls?
Test reagents and machinery needed to do COVID-19 PCR testing have became scarce because of the global pressure to ramp up testing capacity. High-income countries that manufacture these products have been prioritising local demand, affecting access for others, including South Africa. The problem became worse during lockdown, which hit global trade.
Another issue is that COVID-19 PCR tests are imperfect laboratory tools in a pandemic. Technically, they are time consuming. It can take from 10 to 24 hours to get results. This has been stretched even further because laboratories have become overloaded, accumulating a backlog of samples.
PCR tests require specialised equipment and highly trained staff. And importantly, they are primarily designed to be diagnostic in individuals with symptoms. But these tests perform poorly when applied to screening of individuals who don’t yet have symptoms or those who may never develop symptoms but may still be infected (asymptomatic infections).
The tests may give false negative results in people that are actually infected. This occurs in up to 20% of COVID-19 PCR tests.
Factors that affect the results are the timing of the sample – too early during or too late after infection – and the type and technique used to collect the sample.
What are the alternatives?
Tests that detect SARS-CoV-2 antibodies can be used to supplement laboratory testing and fill in the gaps because of the characteristics of COVID-19 PCR tests. PCR tests detect the actual virus in a throat swab and antibody tests detect the person’s immune response to the virus.
Antibody tests have been successfully implemented in the US, UK, France and Germany as useful laboratory tools to supplement COVID-19 PCR tests.
The appearance of antibodies with viral infections usually follows the same pattern. But with COVID-19, this sequential appearance of antibodies is not consistent. Research suggests that the window period for this test is 10-14 days from symptom onset to the detection of antibodies. This means that antibodies can only be detected by antibody tests about two weeks after infection.
The unusual immune response has led to a reluctance to use antibody tests. This is because it’s currently unknown whether IgG antibodies that are detected by antibody tests indicate immunity to re-infection – or for how long protection from re-infection may last.
An added complication is that there are many types of tests. For example, there are different types of blood tests for antibodies. These include lateral flow tests or finger prick point of care, and enzyme linked immunosorbent or chemiluminescence immunoassays. All indirectly measure exposure or infection by detecting antibodies produced in the normal immune response to a viral infection.
Only antibody tests done by laboratory professionals, in accredited and certified laboratories, with strict quality protocols in place have sufficiently good performance at this time.
Antibody tests have been developed to complement the existing standard PCR test for diagnosis. They can assist in identifying individuals who are asymptomatic but are nevertheless infected with SARS-CoV-2.
Antibody tests are important in epidemiological investigations to describe the extent or prevalence of infection.
What’s your recommendation?
Detection of SARS-CoV-2 antibodies confirms exposure to the virus. But it does not mean the person is immune and protected from re-infection. This shows that COVID-19 antibody tests can’t replace the use of PCR tests in people who have symptoms.
But they can be useful for a host of reasons. These include:
- confirming infection in individuals who have a clinical illness that is suggestive of COVID-19 but who have received a negative PCR result.
- identifying individuals who have been exposed to SARS-CoV-2 who can donate their blood to be used as a possible treatment for critically ill people with COVID-19.
- in vaccine trials. An antibody test is the single most important measurement to determine if an experimental COVID-19 vaccine, such as the one being tested in South Africa, works or not. Testing for the antibody enables researchers to see which participants have been exposed to the virus.
- in determining the extent of the epidemic. For example, they can be used to investigate outbreaks of COVID-19 in communities, or in healthcare workers or other workplaces or schools.