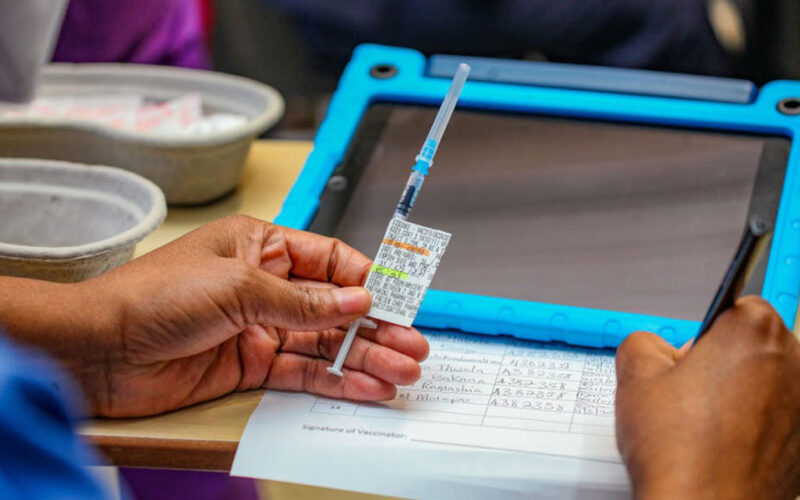
SOUTH Africa has begun the second phase of its public vaccination campaign, targeting people aged 60 or older. The first vaccinations were given in February to health workers. So far almost 600,000 healthcare workers and members of the public have been vaccinated.

Healthcare workers have received the Johnson & Johnson vaccine, while the Pfizer vaccine is being rolled out as part of Phase 2 for members of the public.
A crucial aspect of the vaccination campaign is tracking adverse reactions.
It’s imperative that all health events after vaccination are investigated. All vaccines (and medicines) have side effects. Globally it’s acceptable that some mild and short-lasting symptoms following vaccination may happen. But moderately severe and severe side effects aren’t acceptable. These need to be fully investigated to understand whether the vaccination was responsible.
It’s also important to investigate these events to build trust. If the public understands that all adverse effects following immunisation are taken seriously, and appropriate action is taken, people will have more trust that vaccines are safe.
There has been intense scrutiny of vaccines approved for use against COVID-19. Each has been shown to have different effects – some more serious than others. Most reactions have been mild, going away within a few days on their own. These include mild fever or pain or redness at the injection site. Other side effects include high fever, fatigue, headache, muscle pain, rash at the injection site, chills, and mild diarrhoea.
Allergic reactions are also not uncommon. These are usually mild, but can be severe, though this isn’t common. A severe allergic reaction, known as anaphylaxis, can lead to low blood pressure, collapse, difficulty breathing or skin rash. This needs emergency treatment.
More serious or long-lasting side effects to vaccines have been reported, but they’re extremely rare. One is a condition known as vaccine-induced thrombosis and thrombocytopenia – blood clots together with low platelets. Symptoms appear between 10 and 14 days after vaccination. Just six cases of the rare clots – in more than 6.8 million doses of the Johnson & Johnson vaccine – were reported by the US Food and Drug Administration.
The World Health Organisation (WHO) has been supporting low and middle-income countries to establish immunisation safety expert committees and other structures to better detect, report and analyse adverse events. This is part of the Global Vaccine Safety Blueprint.
In South Africa, the Minister of Health set up the National Immunisation Safety Expert Committee to investigate and report on adverse effects following immunisation. Until now, the work of the committee has focused on adverse events reported after routine childhood vaccines. SARS-CoV-2 is the first vaccine routinely administered to adults. This has required an expansion of the committee to include people with the right skills.
My insights are gained from being a member of the committee and a public health professional. There is a great deal of anxiety about the safety of vaccines. By fully investigating and understanding adverse events following vaccination, South Africa will not only build trust in vaccine safety. It will also contribute valuable evidence towards global vaccine development.
Investigating adverse effects
Each province and district in South Africa has allocated people responsible for investigating adverse events following vaccination. They usually belong to the Expanded Programme of Immunisation team or the communicable disease surveillance team.
But any health practitioner or member of the public can report an adverse event. This can be done through a ‘MedSafety App’ or by completing a ‘case report form’.
Once the provincial or district teams have been given the medical records of the person who experienced the adverse event, they submit these to the national immunisation safety expert committee. This committee is appointed by the Minister of Health and includes experts from all clinical disciplines including pharmacists, infectious disease specialists, paediatricians and pathologists.
The committee uses an algorithm created by the World Health Organisation (WHO) to examine what is reported about the event. This includes the patient’s clinical details and standard case definitions.
When all the data is put together, the committee categorises the event as being:
- ‘consistent with a causal association to immunisation’ (caused by the vaccine). This includes reactions related to a defect in the vaccine and anxiety-related reactions
- a co-incidental event
- temporally associated with vaccination but without definitive evidence that the vaccine caused the event
The committee reports its findings to the Minister of Health, the National Department of Health and the Provincial Departments of Health. Adverse event data and final assessments are then reported into the WHO so that pooled data from countries can contribute to global monitoring of safety signals.
Safety data from vaccine trials has provided sufficient data that vaccines are generally safe. However vaccine trials do not have sufficient numbers of people to detect rare events. Monitoring of vaccines adverse events at country or global level will allow rare events to be detected. If detected, decisions need to be made regarding risk-benefit ratios to decide if the vaccine should continue to be used.
Recourse
All COVID-19 vaccines currently administered are made available through the WHO’s emergency use assessment and listing procedures. These set out how health products should be evaluated for performance, quality and safety in truncated timelines.
However, because these are new products, there may be risks. The WHO has therefore advised countries to ensure fair compensation through creation of ‘no fault compensation schemes’. This allows for a payout without the need to go to court to establish who was responsible (hence ‘no fault’). This makes the compensation process faster and cheaper.
The WHO has provided funds for countries that are beneficiaries of COVID-19 vaccines through subsidised schemes. South Africa is not eligible for this. The government is therefore required to create its own compensation programme.
Details of how the South African ‘no fault compensation process’ will work are being finalised in new legislation being drawn up. The idea is that individuals who suffered an adverse event would be able to receive monetary compensation following review and investigation of the case.