CERVICAL cancer is the second most common cancer among women in Nigeria. There were 31,955 new cervical cancer cases in West Africa in 2018, and Nigeria accounted for almost half (14,943). There were also 10,403 deaths (28 deaths every day) from cervical cancer in the country in the same year.

About 70% of all cervical cancer cases are caused by human papillomavirus (HPV) serotypes 16 and 18. The most common mode of transmission is through sex, but it can also be transmitted through the use of contaminated hospital equipment and from mother to child. Cancer is ranked second in the number of years lost to disability among women in Nigeria.
There are screening programmes geared towards the prevention of this cancer, including Papanicolaou (Pap) smear and HPV screening. These are secondary preventive measures that detect early-stage cervical cell abnormality and the virus’s presence. However, only 8.7% of Nigerian women had a pap smear in 2018, and fewer had HPV screening.
This low uptake results from poorly organised services, the relatively high cost, and the shortage of resources and skills required for the services.
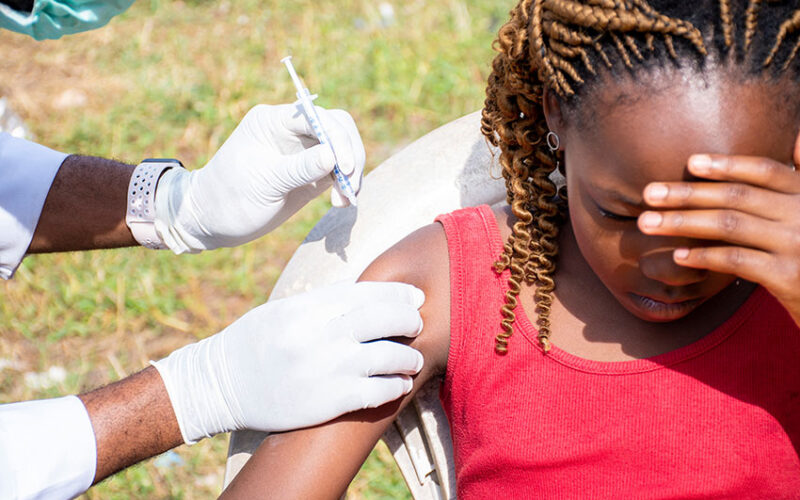
The HPV vaccine is an effective primary prevention measure for cervical cancer. The vaccine is most effective when started before sexual debut, which is the reason for the recommendation of its administration in early adolescence.
There are, however, two main obstacles on this path. First, the vaccine is currently being marketed at exorbitant costs. It is therefore out of reach of the average family. The Nigerian government is seeking ways to meet the conditions for accessing subsidised HPV vaccines under the global assistance programme.
Second, Nigeria is yet to identify an organised structure through which most of the eligible adolescents can be reached with the HPV vaccine. A multi-pronged approach will be required for this as many Nigerian adolescents are out of school.
Case for early vaccination
The HPV vaccine has been introduced in some African countries. But it is yet to be integrated into the routine vaccine schedule in Nigeria. Part of the preparation to ensure the successful introduction of the HPV vaccine is to ensure that all stakeholders have correct perspectives about the vaccine.
Vaccinating both girls and boys has been shown to be more cost-effective because it can lead to the development of herd immunity, curbing the spread of the virus, and prevent other HPV-related cancers like anogenital cancers and cancer of the head and neck.
Parents are essential stakeholders in the HPV vaccine programme for adolescents because they are the primary caregivers. They will play significant roles in the decision making process for the uptake of HPV vaccination. If Nigeria uses the school-based or community-based HPV vaccination programme, parents’ consent is crucial for the success of the programme.
The importance of parental consent was emphasised by the parents of adolescents that we interviewed in five selected communities in Ibadan, a city home to 3.5 million in southwest Nigeria. This is not only right legally as these adolescents are minors, but the parents are their primary caregivers. They should be involved in decisions about the uptake of healthcare services, including HPV vaccination.
Almost all the parents we spoke to had the intention to vaccinate their adolescents with the HPV vaccine despite being informed that the virus was sexually transmitted. However, parents who were older than 45 years were reluctant to vaccinate their adolescents. Findings from this study showed that many parents in this age group did not believe that HPV was responsible for cervical cancer and did not appreciate the importance of the HPV vaccine in preventing cancer. Also, these older parents significantly did not have formal education. Older people have been reluctant in the uptake of new technology, which might have affected these parents’ views about the HPV vaccine.
Way forward
It is essential to carry all stakeholders along in this pre-introduction era of the HPV vaccine in Nigeria to ensure the programme’s success in the future. A concerted effort is required to demonstrate the relationship between HPV and cervical cancer and the role of the vaccine in the prevention of cancer.
This will require special health education skills as most of the parents do not have formal education. All parents should also be involved at each stage of the introduction of the HPV vaccine for the programme to succeed.
The HPV vaccine offers hope for a world free from cervical cancer, and the HPV infection can be curtailed if herd immunity is achieved using the vaccine. This can be achieved with the cooperation of parents, leaving no one behind.